Is Intermittent Fasting Healthy? Evidence-Based Answer
Intermittent fasting can be healthy for some people, but not for everyone. That’s the short answer.
The real question is: healthy for whom, under what conditions, and compared with what? If you judge intermittent fasting (IF) only by social media claims, you’ll get extreme answers. If you judge it by evidence quality, the picture gets clearer.
This guide breaks down what stronger studies say, where the risks are real, and how to decide if IF is a good fit for your health.

Quick Context: What Intermittent Fasting Is (Brief)
Intermittent fasting means cycling between eating windows and fasting windows. Common formats include 16:8 (fast 16 hours, eat within 8), 5:2 (eat normally 5 days, lower-calorie intake 2 days), and alternate-day fasting.
Important point: IF is a meal-timing strategy, not a magic metabolic switch. In many real-world cases, people lose weight because IF helps them reduce total calorie intake and late-night snacking.
Is Intermittent Fasting Healthy? Start with Evidence Quality
When people ask “is intermittent fasting healthy?”, they often mix very different types of evidence:
- Randomized controlled trials (RCTs) and meta-analyses (generally stronger)
- Observational studies (useful, but more confounding)
- Conference abstracts/news headlines (early signals, not final conclusions)
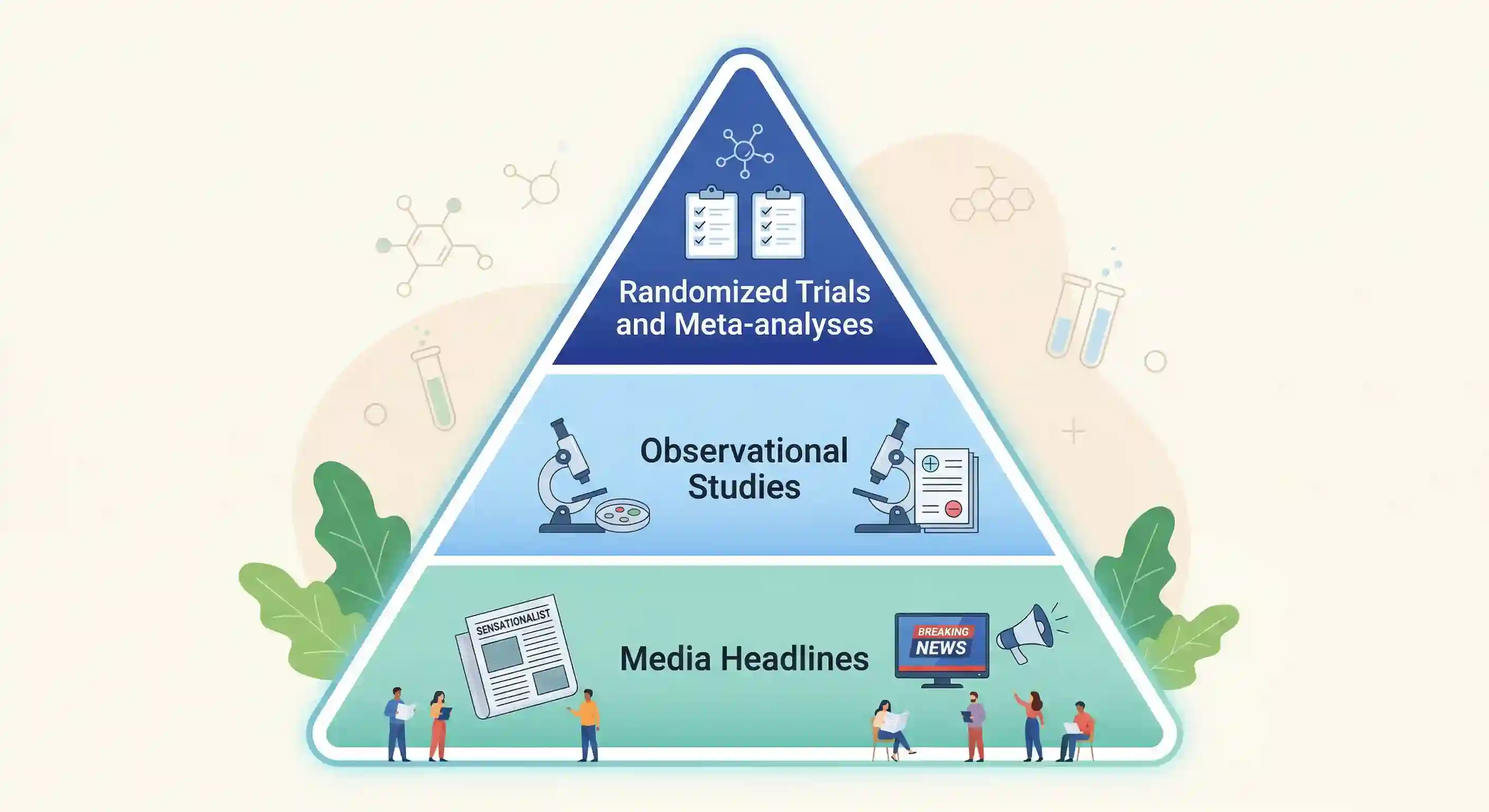
That difference matters.
For example, one high-profile 2022 NEJM RCT found that under matched calorie restriction, adding time-restricted eating did not produce a significantly greater weight-loss benefit than calorie restriction alone (NEJM, PubMed). This does not mean IF is “bad.” It means IF may be one workable tool, not always a superior one.
Now compare that with attention-grabbing headlines about large cardiovascular risk increases from narrow eating windows. Some of those reports are based on observational analyses presented in conference contexts and should be interpreted cautiously, especially before peer-reviewed full publication and full confounder analysis (AHA summary).
So the first healthy decision is this: don’t treat all evidence as equal.
When IF Looks Healthy: What Benefits Are Realistic
Across systematic reviews and meta-analyses, intermittent fasting often shows modest benefits in the right populations—especially adults with overweight, obesity, prediabetes, or type 2 diabetes (longer-term meta-analysis, umbrella review).
1) Weight and waist outcomes
IF can help reduce body weight and central adiposity in many studies. The key word is can. Results vary based on adherence, baseline diet quality, sleep, activity, stress, and medication context.
2) Metabolic markers
Some studies suggest improvements in fasting glucose, insulin sensitivity, blood pressure, or lipid markers in selected groups. But these are not guaranteed, and magnitude differs across protocols and populations.
3) Why people feel it works
For many people, IF simplifies decision-making:
- fewer eating opportunities
- less late-night grazing
- clearer structure
That behavioral simplicity can be a genuine health advantage if it improves long-term consistency.
In plain language: IF can be healthy when it helps you sustain a nutritious calorie pattern without causing physical or psychological harm.
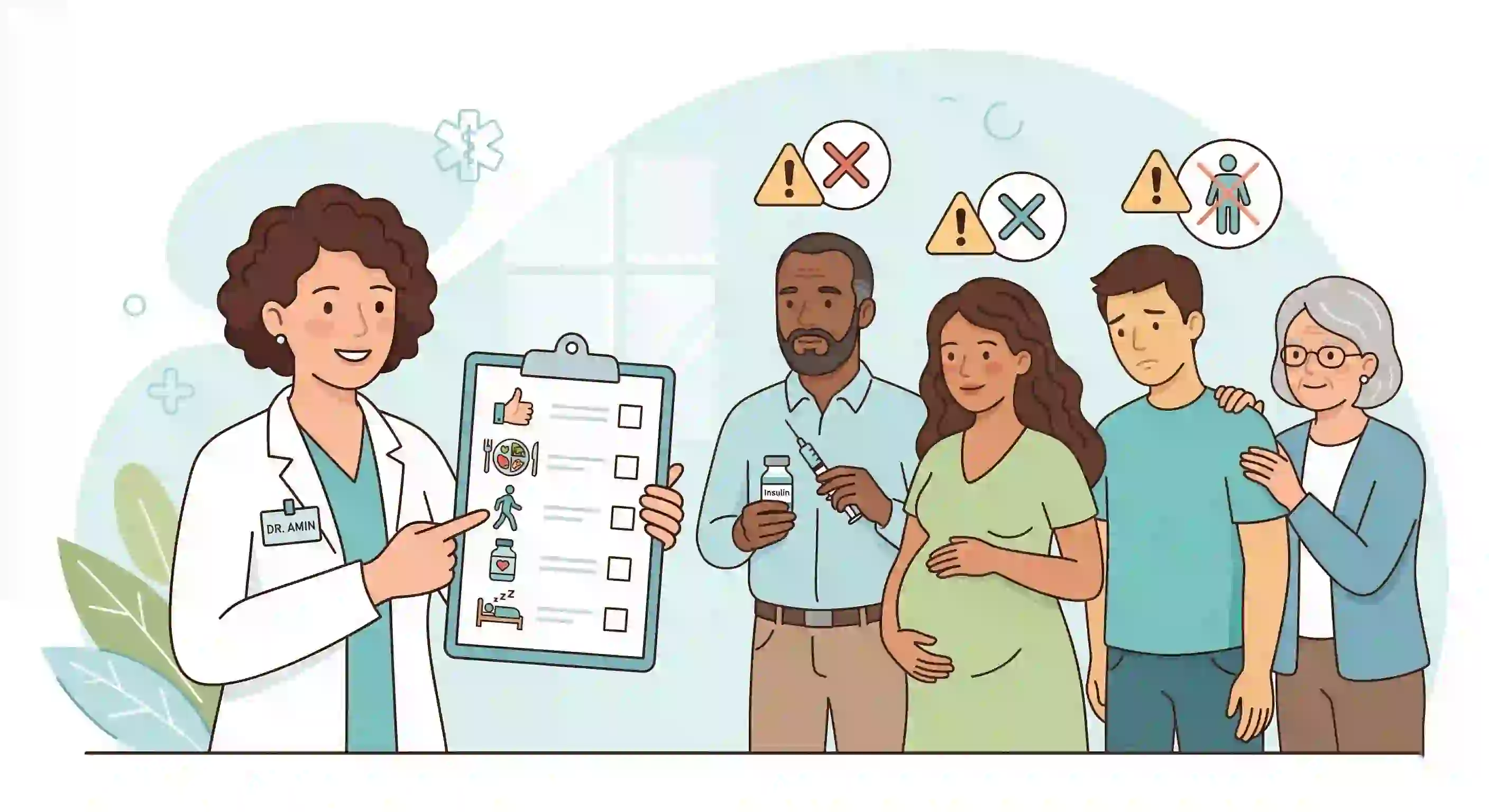
When IF May Not Be Healthy
Intermittent fasting is not universally safe. In some contexts, it can raise risk.
1) Diabetes medications and hypoglycemia risk
If you use glucose-lowering medications (especially insulin or sulfonylureas), fasting can increase hypoglycemia risk unless medication timing/dose is medically adjusted. NIDDK emphasizes planning fasting with clinical supervision in diabetes contexts (NIDDK guidance).
2) Pregnancy and breastfeeding
Pregnancy and breastfeeding are special metabolic states. Restrictive fasting patterns can be inappropriate depending on individual nutritional needs and clinical context. If this applies to you, start here for focused context: Intermittent Fasting While Breastfeeding.
3) Eating disorder history or high food preoccupation
If fasting windows trigger binge-restrict cycles, anxiety, or obsessive food behavior, IF is likely not healthy for you right now.
4) Other caution groups
You should seek medical clearance before trying IF if you are:
- underweight or medically frail
- on complex medication regimens
- managing chronic disease with unstable symptoms
- experiencing recurrent dizziness, fatigue, or sleep disruption
A strategy is only “healthy” if your whole system tolerates it.
Is IF Healthier Than Regular Calorie Restriction?
Usually, the best evidence says: not necessarily.
When calorie intake and support are controlled, IF often performs similarly to standard calorie-restriction approaches for weight loss and several metabolic outcomes.
That means your best diet framework is often the one you can maintain safely and consistently.
So instead of asking, “Is IF superior?” ask:
- Does this pattern improve my health markers?
- Can I sustain it without side effects?
- Does it reduce decision fatigue and overeating?
- Is my relationship with food staying stable?
If those answers are mostly yes, IF may be healthy for you.
Health-First Decision Checklist (Try / Try Carefully / Avoid)
Use this practical filter before you start.
Try (generally reasonable)
- You are an adult without major contraindications
- You can maintain hydration, protein intake, and sleep
- You want a simple structure for appetite/meal timing control
Try Carefully (monitor closely)
- You have a history of blood sugar variability
- You have high training demands and recovery concerns
- You notice mood, sleep, or menstrual-cycle disruption
Avoid for now (or get clinician guidance first)
- Pregnancy or breastfeeding
- Eating disorder history
- Diabetes on medications with hypoglycemia risk without a supervision plan
- Any condition where fasting may destabilize treatment
A low-risk 2–4 week trial framework
- Start with a gentler window (for example, 12:12 then 14:10).
- Keep protein and hydration consistent.
- Track energy, sleep, hunger, mood, training performance, and concentration.
- Reassess weekly. If red flags appear, stop and adjust.
If you want better adherence, use a real-time tracker that shows elapsed time, target end time, and reminders, and keeps your fasting history in one place: Intermittent Fasting Timer.
Red flags that mean “pause now”
- repeated dizziness or near-fainting
- severe irritability, poor concentration, or insomnia
- binge-restrict patterns
- persistent fatigue and performance drop
- symptoms of hypoglycemia
When those appear, “pushing through” is usually not a health win.
Bottom Line: Is Intermittent Fasting Healthy?
Intermittent fasting can be healthy, conditionally healthy, or unhealthy—depending on your context.
It tends to be most helpful when it improves consistency in eating patterns, supports sustainable energy balance, and does not create medical or behavioral harm. It is less likely to be healthy when done aggressively, without risk screening, or in high-risk groups without supervision.
If you want a practical starting point, use this free tool to choose a fasting method (16:8, 18:6, 14:10, 20:4, or OMAD), set your meal timing, and generate your fasting/eating schedule: Intermittent Fasting Calculator.
The best approach is simple: risk-screen first, start small, monitor response, and adapt.
FAQ
Is intermittent fasting healthy for women?
It can be, but your life stage matters more than the protocol label. Women in high-stress periods, with poor sleep, or with high training loads are often more sensitive to aggressive fasting windows. A practical approach is to start with a mild window and watch cycle regularity, recovery, and mood. If those worsen, scale back or stop. The right plan is the one your body tolerates well over time.
Is intermittent fasting safe for people with diabetes?
It can be done in some cases, but it should be treated as a medically guided change, not a lifestyle experiment. The main issue is glucose variability and hypoglycemia risk when medication and meal timing no longer match. Before starting, align on a monitoring plan, medication plan, and stop rules with your clinician. Without that setup, the risk-benefit balance is usually poor.
Can intermittent fasting slow metabolism?
IF itself is not a guaranteed metabolic problem. What usually causes trouble is running too large a deficit for too long, then seeing energy, movement, and training quality drop. If your routine becomes hard to sustain, total daily expenditure can fall and progress stalls. In practice, consistency, sleep, and adequate nutrition matter more than fasting window length alone.
Will intermittent fasting cause muscle loss?
It can if your overall setup is weak, especially when protein intake is low and resistance training is missing. But with regular strength work and sufficient protein, many people maintain lean mass while using IF. Think of fasting as a schedule tool: muscle outcomes still depend on training stimulus and total nutrition across the week.
How long should I test intermittent fasting before deciding if it works for me?
Use a short evaluation cycle, then decide with objective criteria. Two to four weeks is enough for a first pass. Define success in advance: better adherence, stable energy, manageable hunger, and no meaningful decline in sleep or performance. If you only lose structure and feel worse, that is a valid signal to switch methods.
What are warning signs I should stop intermittent fasting?
Treat persistent functional decline as your stop signal. If fasting repeatedly causes dizziness, poor concentration at work, sleep disruption, irritability, or rebound overeating, it’s not a good fit right now. One bad day is normal; repeated patterns are the issue. In diabetes or other high-risk conditions, follow your medical stop criteria immediately.
Read More
How to know your ideal fasting time?

Find your ideal fasting window with a practical 2-week method. Learn when to choose 14/10 or 16/8, what signals to track, and when to adjust safely
Read moreWhat are the basic rules for intermittent fasting?

Unlock your best self! Discover essential intermittent fasting rules to boost energy, weight loss, and simplify healthy living.
Read moreUltimate Guide to Intermittent Fasting While Breastfeeding

Is intermittent fasting safe while breastfeeding? Complete medical guide covering risks, benefits, and safe approaches for mothers. Expert advice included
Read more